Noticing blood in your stool or vomit is frightening — and your instinct to look for answers right away is exactly right. Gastrointestinal (GI) bleeding in adults is a symptom that can range from a minor nuisance to a serious medical emergency. Understanding what causes gastrointestinal bleeding in adults is the first step toward getting the care you need quickly and safely.
In this guide, we break down the most common causes, the warning signs you should never ignore, how doctors diagnose the problem, and what treatment options are available — explained in plain, easy-to-understand language.
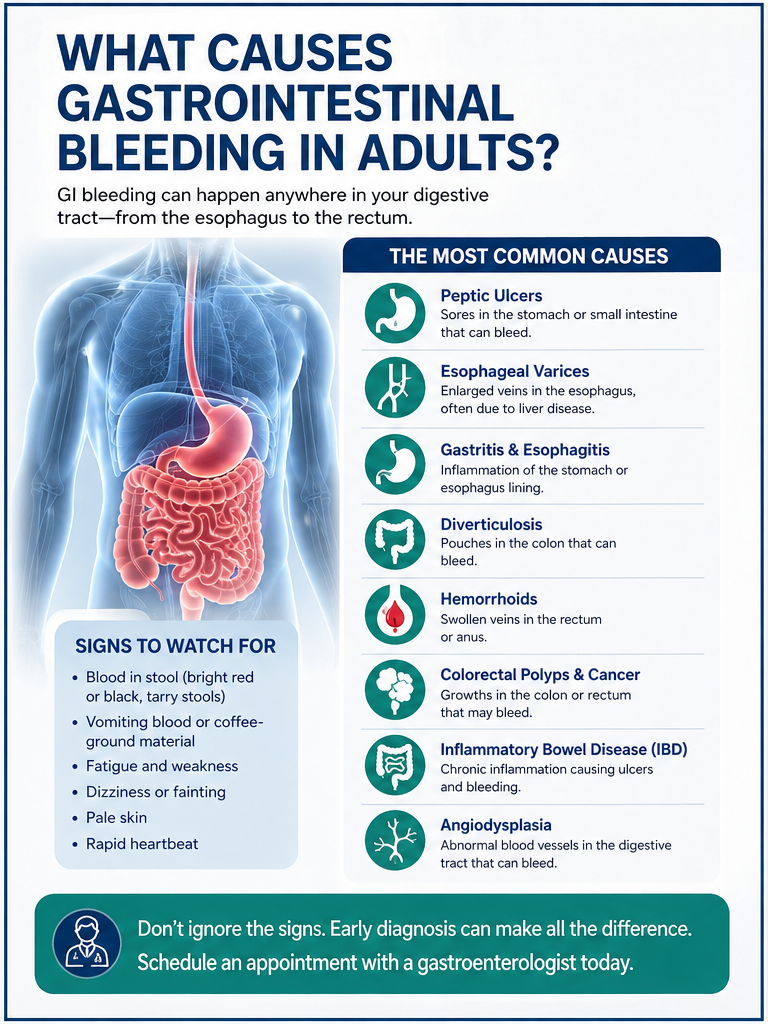
| Quick Answer GI bleeding in adults is most often caused by peptic ulcers, hemorrhoids, diverticulosis, inflammatory bowel disease, or colorectal polyps and cancer. It can originate anywhere in the digestive tract — from the esophagus all the way to the rectum. |
What Is Gastrointestinal Bleeding?
Gastrointestinal (GI) bleeding refers to any bleeding that occurs within the digestive tract — the long system of organs that runs from your mouth to your anus, including the esophagus, stomach, small intestine, large intestine (colon), and rectum.
Doctors classify GI bleeding into two main categories based on where it originates:
Upper GI Bleeding vs. Lower GI Bleeding Symptoms
Upper GI bleeding comes from the esophagus, stomach, or the first part of the small intestine (duodenum). Lower GI bleeding originates from the colon, rectum, or anus. Knowing the difference helps doctors find the source faster.
| Upper GI Bleeding | Lower GI Bleeding |
| Dark, tarry black stools (melena) Vomiting blood or coffee-ground material Stomach pain or burning | Bright red or maroon blood in stool Blood on toilet paper or in toilet bowl Rectal pain or pressure |
Signs of Internal Bleeding in the Digestive Tract
Not all GI bleeding is visible to the naked eye. Sometimes it is called “occult” bleeding — meaning it can only be detected through lab tests. Here are the most common signs of internal bleeding in the digestive tract:
- Fatigue and weakness: ongoing blood loss causes anemia, making you feel exhausted even without obvious bleeding
- Pale or yellowish skin: a sign that your red blood cell count has dropped
- Shortness of breath: less oxygen-carrying capacity in your blood
- Dizziness or fainting: especially when standing up quickly
- Rapid heartbeat: your heart works harder to compensate for blood loss
- Black, tar-like stools: often a sign of slow bleeding from the upper GI tract
If you notice any of these signs alongside changes in bowel habits, schedule an appointment with a gastroenterologist promptly.
The Most Common Causes of GI Bleeding in Adults
Several conditions can trigger gastrointestinal bleeding. Here is a clear breakdown of the most common causes, organized from upper to lower GI tract.
1. Peptic Ulcers — Gastrointestinal Bleeding Risk Factors
Peptic ulcers are open sores that form on the lining of the stomach or small intestine. They are one of the leading causes of upper GI bleeding. The main peptic ulcer gastrointestinal bleeding risk factors include:
- Infection with H. pylori bacteria
- Long-term use of NSAIDs (aspirin, ibuprofen, naproxen)
- Excessive alcohol consumption
- Smoking
Chronic stress — though stress alone rarely causes an ulcer, it can worsen symptoms
2. Esophageal Varices
These are enlarged veins in the esophagus, usually caused by liver disease (such as cirrhosis). When they rupture, they can cause sudden, severe upper GI bleeding — this is a medical emergency requiring immediate care.
3. Gastritis and Esophagitis
Inflammation of the stomach lining (gastritis) or the esophagus (esophagitis) can cause the lining to become raw and bleed. Common triggers include alcohol, NSAIDs, acid reflux, and certain infections.
4. Diverticulosis
Tiny pouches (diverticula) can form in weak spots along the colon wall. Most people have no symptoms, but when a blood vessel near one of these pouches ruptures, it causes sudden, painless lower GI bleeding — often significant in volume.
5. Hemorrhoids
Hemorrhoids are swollen veins in the rectum or anus. They are one of the most common causes of blood on toilet paper or in the toilet bowl after a bowel movement. While usually not dangerous, persistent hemorrhoid bleeding should be evaluated by a doctor.
6. Colorectal Polyps and Colon Cancer
Polyps are small growths on the inner lining of the colon or rectum. Some polyps are benign; others can develop into colon cancer over time. Both can cause slow, intermittent bleeding that is often invisible without a stool test. This is one key reason why regular colonoscopy screenings are so important.
7. Inflammatory Bowel Disease (IBD)
Conditions like Crohn’s disease and ulcerative colitis cause chronic inflammation in the digestive tract, leading to ulcers and bloody diarrhea. IBD-related bleeding can be mild or severe depending on how active the disease is.
8. Angiodysplasia
Abnormal, fragile blood vessels in the colon or small intestine can bleed intermittently. This is more common in older adults and can be tricky to find without specialized testing
When to Go to the ER for Blood in Stool
| Go to the Emergency Room IMMEDIATELY if you have: • Vomiting blood or material that looks like coffee grounds • Large amounts of bright red blood from the rectum • Black, tarry stools with dizziness, fainting, or rapid heartbeat • Severe abdominal pain combined with bleeding • Signs of shock: pale skin, rapid breathing, confusion, or loss of consciousness |
How Is GI Bleeding Diagnosed? Endoscopy vs. Capsule Endoscopy
Getting an accurate diagnosis is essential. Your gastroenterologist will use one or more of the following tools to identify the source of bleeding:
Upper Endoscopy (EGD)
A thin, flexible tube with a camera is passed through your mouth into the esophagus, stomach, and upper small intestine. This is the gold standard for diagnosing upper GI bleeding. It can also treat the bleeding source in the same procedure.
Colonoscopy
A colonoscopy uses a similar flexible scope inserted through the rectum to examine the entire colon and rectum. It can identify polyps, ulcers, cancer, diverticulosis, and sources of lower GI bleeding — and treat some of them on the spot.
Capsule Endoscopy
You swallow a small, pill-sized camera that transmits images as it travels through your digestive tract. This is particularly useful for finding bleeding sources in the small intestine that are out of reach for standard scopes — making it a key tool in the endoscopy vs. capsule comparison for small bowel bleeding.
Other Diagnostic Tools
- Stool tests (fecal occult blood test) — detect hidden blood
- CT angiography — locates active bleeding through imaging
- Blood tests — assess blood count, clotting, and liver function
Gastrointestinal Bleeding Treatment Options Without Surgery
The good news is that most GI bleeding can be managed without surgery. Treatment depends on the cause, location, and severity of bleeding:
Endoscopic Treatments
During an endoscopy or colonoscopy, your doctor can often stop the bleeding by:
- Injecting medication directly into the bleeding site
- Using heat (cauterization) to seal the vessel
- Placing clips or rubber bands (for hemorrhoids or varices)
Medications
- Proton pump inhibitors (PPIs): reduce stomach acid to help ulcers heal
- Antibiotics: eliminate H. pylori infection
- Biologics: for inflammatory bowel disease
- Vasopressin or octreotide: for variceal bleeding
Interventional Radiology
For hard-to-reach bleeding, a radiologist can thread a catheter through blood vessels to deliver medication or a blocking agent directly to the source.
Surgery
Surgery is reserved for cases where other treatments have failed, or where the cause (such as advanced colon cancer or a severe perforation) requires it. Advances in endoscopy mean surgery is needed far less often today than it was in previous decades.
GI Bleeding Diet: Foods to Avoid After Diagnosis
After a GI bleeding diagnosis, your doctor will likely recommend dietary adjustments to reduce irritation and support healing. Here are the most important GI bleeding diet foods to avoid:
Foods and Substances to Avoid
- Alcohol — irritates the GI lining and impairs clotting
- Spicy foods — can aggravate inflammation and ulcer pain
- Acidic foods (citrus, tomatoes, vinegar) — increase acid in the stomach
- NSAIDs (aspirin, ibuprofen, naproxen) — thin blood and damage the stomach lining; discuss alternatives with your doctor
- Caffeine — stimulates acid production
- Red meat in large quantities — may increase colorectal cancer risk over time
Foods That Support Healing
- High-fiber foods (oats, vegetables, legumes) — reduce constipation and hemorrhoid strain
- Probiotic-rich foods (yogurt, kefir) — support a healthy gut environment
- Lean proteins (chicken, fish, tofu) — help tissue repair
- Water — staying well-hydrated keeps stools soft and reduces straining
Always follow your gastroenterologist’s specific dietary guidance, as recommendations vary depending on the cause and location of your bleeding.
When Should You See a Gastroenterologist?
If you have noticed any blood in your stool, changes in bowel habits, unexplained fatigue, or abdominal pain — even if the symptoms seem minor — it is worth getting a professional evaluation. Early diagnosis almost always leads to better outcomes.
At Colon & Digestive Health Specialists, Dr. Karim Shakoor and our team offer same-day appointments, comprehensive diagnostic services including colonoscopy and upper endoscopy, and a personalized approach to your digestive health. We also serve patients in Rockdale, Newton, Henry, and surrounding counties in the East Atlanta area.
we provide personalized care plans designed to address both digestive health and stress-related triggers.
stress alone is unlikely to cause GI bleeding directly, but it can make existing conditions worse. Stress increases acid production in the stomach, which can aggravate ulcers and acid reflux. Chronic psychological stress has also been linked to flares of inflammatory bowel disease. However, if you are experiencing GI bleeding symptoms, the cause is almost always a physical condition — not stress on its own. A GI specialist can help identify what is really going on.
Not always — but it should never be ignored. A small amount of bright red blood from an anal fissure or hemorrhoid may not be an emergency, but you should still have it evaluated. Dark, tarry, or large-volume bleeding is a red flag that requires immediate attention.
While the same digestive structures are involved, causes differ. In adults, peptic ulcers, diverticulosis, hemorrhoids, and colon cancer are most common. Children are more likely to have bleeding from Meckel’s diverticulum, intussusception, or juvenile polyps. This guide focuses specifically on GI bleeding in adults.
Recovery depends heavily on the cause and treatment. A mild bleed from a peptic ulcer treated endoscopically may resolve within a week. Recovery from surgery for a more serious condition can take several weeks. Your doctor will monitor your blood count and adjust your care accordingly.
